Learn how a Fortune 500 self-insured employer saved $6M annually using hospital price transparency data. Discover how data-driven healthcare insights reduce costs and optimize benefits strategy.
Healthcare / Employee Benefits
Fortune 500 manufacturing company, 80,000+ covered lives (name withheld under NDA)
14 months (ongoing)
$6.2M in first-year plan savings

A Fortune 500 US manufacturing company partnered with Actowiz Solutions to build a custom hospital price transparency data pipeline that unlocked 6 million dollars in first-year health plan savings. The engagement processed CMS-mandated Machine-Readable Files (MRFs) from over 2,100 hospitals and 47 payers, delivered a normalized, employer-specific dataset, and powered downstream benefit design changes — network steering, centers of excellence programs, and reference-based pricing — that reduced healthcare spend by 4.1% in the first full plan year.
This case study documents how hospital price transparency data, when operationalized properly, becomes one of the highest-ROI data investments available to large self-insured employers in America.
The client is a Fortune 500 US manufacturing company with over 80,000 covered lives across their self-insured medical plan. Their annual healthcare spend exceeded $780 million, growing 7-8% annually in the years before the engagement — meaningfully faster than CPI and wage growth.
The Total Rewards team had attempted multiple cost containment initiatives over the prior 5 years:
By 2024, they had exhausted the obvious levers. What they needed was data: objective, granular, facility-level pricing data to identify where their TPA’s negotiated rates were competitive and where they were not.
The 2021 CMS Hospital Price Transparency rule had theoretically made this data available. But practically, the data was unusable — buried in multi-terabyte MRFs across thousands of hospital websites, with inconsistent schemas, decaying URLs, and no centralized registry.
The client needed an expert partner who could turn regulatory compliance files into decision-ready intelligence.
When the client explored the problem space, they quickly understood why their peer companies had largely ignored price transparency data:
A single large payer’s Transparency in Coverage (TiC) file can exceed 1 TB uncompressed. Processing these files at scale requires distributed computing infrastructure most employers don’t have.
CMS provided a recommended schema. Actual hospital and payer compliance varies dramatically — nested JSON, CSV, XML, custom formats, and deviations from the spec are common.
Hospital MRF URLs change without notice. A static list of URLs becomes 30-40% stale within six months without active monitoring.
Raw MRF data contains CPT, HCPCS, DRG, NDC, and revenue codes. Converting these to plain-English service descriptions requires clinical and billing expertise most employers lack.
Despite the CMS mandate, an estimated 30-40% of hospitals are partially non-compliant — missing files, blocked URLs, or data of limited utility. Navigating this requires ongoing effort.
Peer employers who had attempted in-house pipelines reported $800K-$1.5M of engineering cost with limited results. The client wanted to avoid that path.
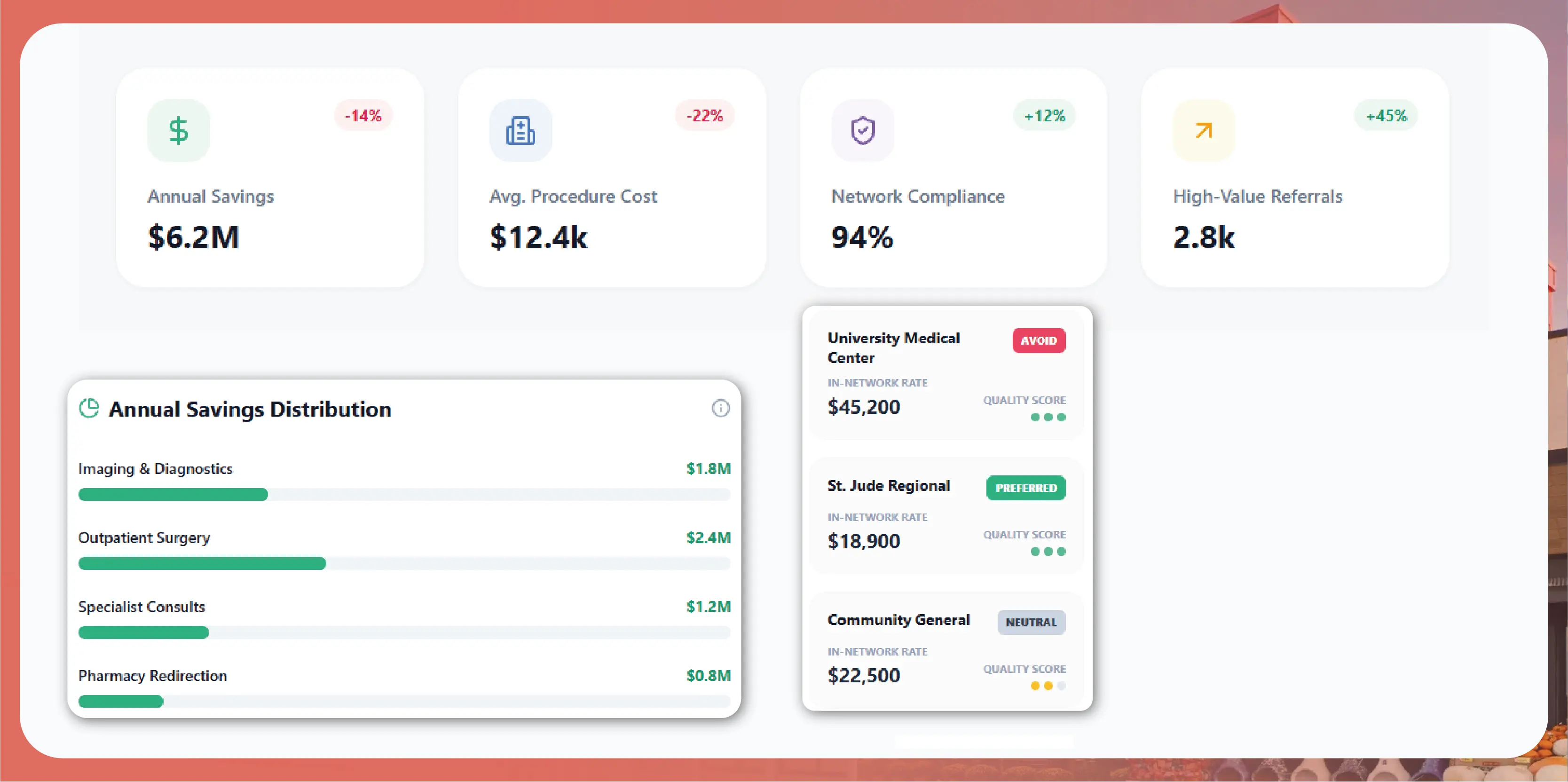
Actowiz designed a turnkey hospital price transparency data platform specifically optimized for large self-insured employer use cases.
Beyond raw data delivery, Actowiz built custom dashboards for the client’s benefits team:
Month 1: Scope definition, facility prioritization, TPA coordination Month 2-3: Initial data pipeline deployment, first hospital set processed Month 4: Full facility coverage achieved, payer TiC processing activated Month 5-6: Normalization, enrichment, and analytics layer deployed Month 7: Benefits team training and initial insights review Month 8: Plan design changes approved by executive committee Month 9-12: Plan year implementation with ongoing data monitoring Month 13-14: First-year results measurement and Year 2 planning
Orthopedic Centers of Excellence Program ($2.4M): The data revealed that knee and hip replacements varied by 35-42% between in-network hospitals in the same metros. The benefits team launched a Centers of Excellence program, steering elective orthopedic procedures to lower-cost, high-quality facilities with bundled pricing. Employee-facing incentives (waived copays, travel reimbursement for distant COE facilities) ensured high adoption.
Imaging Steering ($1.1M): MRI costs varied from $400 to $3,100 across in-network providers for identical procedures. Enhanced benefit navigation tools guided employees to cost-effective imaging centers, reducing imaging spend by 28% with zero quality degradation.
Reference-Based Pricing for Outpatient Surgery ($1.8M): For a specific set of outpatient surgical procedures where the data showed consistent overpayment, the plan introduced reference-based pricing at the 60th percentile of market rates. Legal review ensured compliance; employee communications were managed carefully to limit disruption.
TPA Renegotiation Leverage ($900K): Armed with facility-level comparative data, the benefits team renegotiated specific contract terms with their TPA — eliminating outlier overpayments in 8 facilities where their TPA’s rates were above the 90th market percentile.
The Centers of Excellence (COE) design exemplifies how the data engagement drove specific programmatic decisions.
Step 1: Pricing Discovery Analysis of hospital MRF data across 14 metros where the client had employee concentrations revealed that knee replacement total-episode costs varied from $28,000 to $51,000 across in-network facilities.
Step 2: Quality Filtering The team cross-referenced pricing data with publicly available CMS quality metrics — readmission rates, complication rates, patient satisfaction scores — to ensure steering didn’t sacrifice outcomes.
Step 3: Candidate Facility Identification 24 facilities across the client’s geographies were identified as COE candidates — below 50th percentile pricing AND above 75th percentile quality scores.
Step 4: Benefit Design Employees electing COE facilities received: - Waived in-network deductible - Travel reimbursement up to $1,500 for cross-state COE selection - Concierge benefit navigator support
Step 5: Outcome Measurement In the first plan year: - 41% of elective joint replacements occurred at COE facilities (vs 6% baseline) - Average episode cost decreased 28% - Patient satisfaction scores remained equivalent
Net savings from the program: $2.4M in Year 1, with projected $3.1M in Year 2.
Many employers access raw MRF data but never translate it into plan decisions. The value comes from analytics, not raw files.
The data created opportunities; the benefits team’s careful change management realized them. Employee communications, navigator programs, and incentive design were as important as the underlying data.
Steering purely on cost would have been reputationally and medically risky. Integrating public quality metrics was essential.
The client’s TPA was initially defensive about rate transparency analysis. Building a collaborative working relationship — framing the data as mutual optimization, not adversarial — was critical.
Peer companies who tried to build internal pipelines reported delays, quality issues, and 3-5x higher costs than this engagement.
Actowiz Solutions operates one of the most comprehensive hospital price transparency data platforms in the US. We serve self-insured employers, health plans, healthtech startups, hospital systems, and academic researchers with enterprise-grade MRF discovery, extraction, normalization, and analytics.
Our healthcare data specializations: Hospital Price Transparency (HPT) MRF processing - Transparency in Coverage (TiC) payer file processing - Prescription drug pricing data - Provider directory and credentialing data - CMS quality metrics integration - Geographic and demographic data enrichment
“The data showed us that two in-network hospitals charged 40% different prices for the same orthopedic surgery. Once we saw that, the savings opportunity was undeniable.”
— VP, Total Rewards & Benefits
Our web scraping expertise is relied on by 4,000+ global enterprises including Zomato, Tata Consumer, Subway, and Expedia — helping them turn web data into growth.
Watch how businesses like yours are using Actowiz data to drive growth.
From Zomato to Expedia — see why global leaders trust us with their data.
Backed by automation, data volume, and enterprise-grade scale — we help businesses from startups to Fortune 500s extract competitive insights across the USA, UK, UAE, and beyond.
We partner with agencies, system integrators, and technology platforms to deliver end-to-end solutions across the retail and digital shelf ecosystem.

How healthcare payers, startups, and analysts scrape CMS-mandated hospital price transparency files at scale. Complete 2026 guide to MRF extraction and use cases.
Discover how a Dubai cloud kitchen group saved $2.1M annually and scaled to 80+ virtual brands using Talabat and Careem food intelligence. Learn how data-driven insights optimize menus, pricing, and growth.
Track UK Grocery Products Daily Using Automated Data Scraping across Morrisons, Asda, Tesco, Sainsbury’s, Iceland, Co-op, Waitrose, and Ocado for insights.
Whether you're a startup or a Fortune 500 — we have the right plan for your data needs.